Diabetic Wound Care
Foot Ulcer Specialist in Orange County
What is a Diabetic Foot Ulcer?
A diabetic foot ulcer is an open wound, sore, or severe scrape that usually happens on the bottom of a diabetic patient's foot. Because of the serious risk of infection, almost 6 percent of patients who develop these foot ulcers end up needing to be hospitalized.
Diabetes is actually the leading cause of foot amputations in the U.S. Nearly 25 percent of patients who develop a foot wound with diabetes might require an amputation later on. In fact, a foot ulcer is the starting point for 85 percent of all diabetes-related amputations. Because these numbers are so high, working with a good podiatrist is the best way to heal existing wounds and prevent them from coming back.
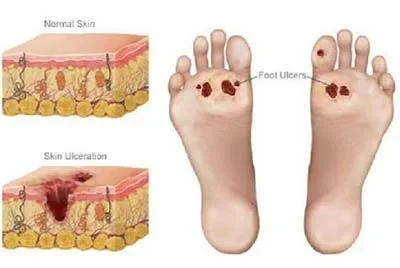
What Causes Foot Ulcers?
Patients with diabetes are much more likely to develop foot wounds. The people at the highest risk tend to be older men, those who use insulin, and patients who also have diabetes-related kidney, eye, or heart disease. African American, Native American, and Hispanic populations also face higher risks. Lifestyle factors like alcohol consumption, smoking, and obesity heavily contribute to ulcer development as well.
Ulcers are usually caused by a perfect storm of issues: how long you've had diabetes, foot trauma, poor blood circulation, foot deformities, and numbness. This numbness is called neuropathy, a condition caused by nerve damage from long-term high blood sugar.
Neuropathy happens silently. Because you lose the ability to feel pain, you might step on something sharp or get a blister from tight shoes and not even realize it until it becomes an ulcer. To check for this, your podiatrist will use a simple, painless tool called a monofilament to test the feeling in your feet.
If a patient also has vascular disease (poor circulation), it makes it much harder for the body to heal the wound and increases the risk of infection. At the same time, high blood sugar weakens the immune system, making the healing process even slower.
Symptoms to Watch For
Because of nerve damage, pain is usually not a reliable symptom. Instead, you need to look for visual signs. The most noticeable clues that an ulcer is forming include drainage or spots on your socks, swelling in the foot, unusual odors, and redness on the skin.
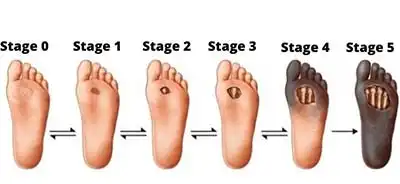
When to See a Specialist
The exact moment you notice an ulcer, you should seek out a diabetic wound care specialist in Irvine. Waiting increases the risk of serious infection and amputation. Getting treatment immediately will keep your feet healthier and lower your overall healthcare costs.
Diagnosis, Treatment, and Care
Healing the wound as rapidly as possible is our main goal. The faster it closes, the lower your chance of infection. A proper treatment plan from your podiatrist will include:
- Infection Prevention: Keeping the area clean and monitoring for any signs of spreading bacteria.
- Off-loading: Taking the pressure off the wound area so it can heal.
- Debridement: Carefully removing the dead skin and tissue around the wound.
- Proper Dressing: Applying medical-grade bandages and treatments.
- Blood Glucose Management: Working to keep your blood sugar at a healthy level.
If your podiatrist finds that the ulcer is infected, they will prescribe an antibiotics plan. For severe cases, specialized wound care or even hospitalization may be arranged.
How Off-Loading Works
"Off-loading" is highly recommended for ulcers on the bottom of the foot. It simply means taking the weight off the wound. Your podiatrist might prescribe crutches, a specialized cast, a brace, a wheelchair, or special footwear. This stops the friction and pressure that makes ulcers worse, allowing rapid recovery.
Proper Wound Dressing at Home
The golden rule for wound care is to keep the ulcer covered and protected from moisture and dirt. However, you must avoid home remedies that can damage healing skin. Do not use hydrogen peroxide, strong betadine, saltwater soaks, or whirlpools.
Instead, your podiatrist will prescribe safe, advanced materials like normal saline, stem cell dressings, growth factor dressings, skin substitutes, and topical medications. Keeping your blood sugar controlled during this time is the most important thing you can do to help the medicine work.

Surgical Options
If your foot ulcer isn't infected, it can likely be treated without surgery. However, if conventional methods aren't working or the infection is severe, surgery might be the best option. This can include removing infected bone, or correcting bunions and hammertoes that are causing dangerous pressure on the area. Recovery time ranges from a few weeks to a few months depending on the surgery.
Preventive Ulcer Care
The absolute best way to treat a foot ulcer is to stop it from developing in the first place. Regular visits to your podiatrist are highly recommended to check if you are a high-risk candidate. You are at high risk if you have:
- Neuropathy (loss of feeling)
- Poor blood circulation
- Foot deformities like bunions or hammertoes
- A habit of wearing inappropriate or tight shoes
- High blood sugar levels
- A past history of foot ulcers
To protect yourself, avoid smoking and heavy drinking, and manage your cholesterol and blood sugar. Wearing special shoes and socks prescribed by your podiatrist will greatly reduce your risk.
Check your feet every single day. Look closely between your toes for cracks, blisters, cuts, bruises, or anything abnormal. Every time you visit the podiatrist, take your shoes and socks off so the doctor can examine you. If you spot a problem at home, report it immediately—no matter how small it seems.

Quick Reference FAQs
Schedule Your Evaluation Today
If you are looking for a diabetic wound care specialist in Irvine, contact our Orange County wound care center at 4330 Barranca PKWY Suite 101, Irvine, CA.
Schedule an Appointment Call (949) 786-7114Our Podiatry Services
Comprehensive Care For Your Foundation
With more than 20 years of experience treating patients with complex foot and ankle problems, we are proud to be one of the most reliable podiatry clinics in Irvine, California.
Toenail Laser Treatment
With our state-of-the-art laser equipment, we can help clear your nails. Ask about our 10% off promotion.

Stem Cell Therapy
Advanced regenerative medicine designed to treat joint degeneration, inflammation, and chronic pain without surgery.

Custom Orthotics
Our comprehensive podiatric system includes custom foot orthotics to correct mechanics and provide stronger pain relief.
Why Choose Us?
Over 20 Years of Clinical Excellence
You may be surprised to know that your feet are not supposed to hurt. If you are experiencing daily foot pain, you are not alone; nearly sixty percent of the population seeks help for a foot problem every year. If you are looking for a trusted specialist in Orange County, we are here to help you get back to a pain-free life.
20+ Years Podiatry Experience
State-of-the-Art Technology
Unmatched Patient Satisfaction
